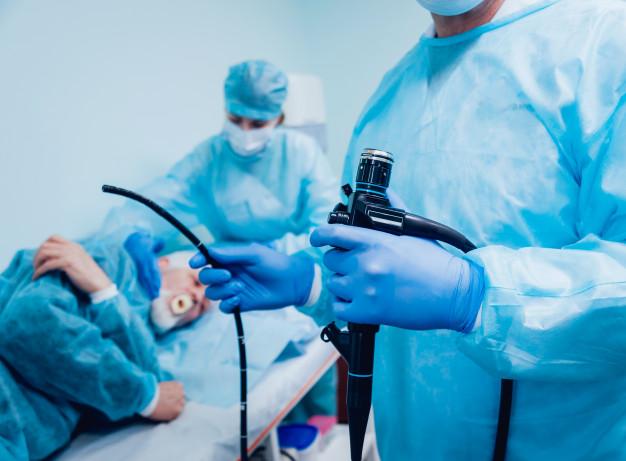
Surgical gastroenterology is a speciality that deals with the treatment and management of diseases related to the gastrointestinal tract. This includes organs such as the stomach, pancreas, small and large intestine, oesophagus, liver, rectum, anus, bladder and biliary tract.
The Department of Surgical Gastroenterology at Ananya Hospital is composed of some of the top surgical gastroenterologists in Hyderabad. Our team of highly skilled and experienced doctors have the ability and expertise in treating and managing all gastrointestinal, liver and pancreaticobiliary diseases.
The doctors at Ananya Hospital have the expertise in the management of disorders like chronic diarrhoea, constipation, peptic ulcer, acute liver failure, portal hypertension, biliopancreatic disorders and malignancies. The high success rate of operations and the dedication of the surgeons in delivering the best care to the patients has helped us gain a reputation as the best gastroenterology hospital in Hyderabad.
With careful analysis of each case, collaboration with other specialists, we have consistently observed a high success rate, even with the most complex surgical procedures. We are equipped with the latest state-of-the-art facilities and surgical equipment. If you are looking for the best Liver transplant surgeon in Hyderabad, look no further, Ananya Hospital is here to help you reclaim your health and well-being.
The Surgical Gastroenterology department is led by the distinguished Dr. Anandakumar, who is renowned in the medical world for his exceptional expertise in surgical gastroenterology. His comprehensive approach in diagnosis, prevention and treatment of diseases is unmatched. Having operated a large number of surgeries, including many complicated ones, Dr.Anandakumar is the very epitome of excellence and dedication.
At Ananya Hospital the highest has and will always be the welfare of the patients. The facilities, doctors and support services are dedicated to providing the finest care for our patients.
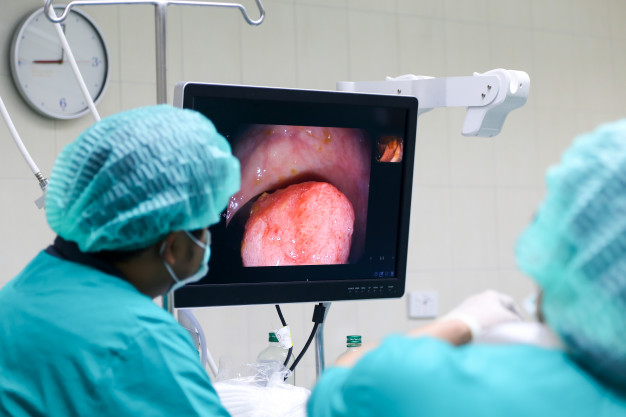 SURGICAL GASTROENTEROLOGY
SURGICAL GASTROENTEROLOGY
- Performing open surgical and keyhole procedures.
- Performing suture-less surgery with Endo GI Staples and bloodless surgery with ultrasonic scalpel.
- Integrating novel healthcare delivery models with innovative clinical and basic research.
- Treating complex gastrointestinal surgical procedures with advanced technology.
- Expertise in hepatobiliary, pancreatic, gastroesophageal, colorectal and surgeries for the small bowel, portal hypertension, spleen and major GI trauma.
UPPER GI SURGERY
- Transhiatal Esophagectomy, Transthoracic Esophagectomy for Esophageal Cancers
- Colon Transposition for Corrosive Esophageal Strictures
- Achalasia Cardia Surgeries
- Radical Gastrectomy for Gastric Cancers
- Radical Hemicolectomies, Anterior Resection
- APR for Cancer of Colon and Cancer of rectum
- Surgery for Retroperitoneal Tumours
LAPAROSCOPIC SURGERIES
- Laparoscopic Cholecystectomy, Appendicectomy, Laparoscopic APR
- Laparoscopic Fundoplication
- Laparoscopic Splenectomy
- Laparoscopic Liver Surgeries
- Laparoscopic Hernia Surgeries
- Single Port Surgeries
- Staples Anopexy (MIPH for piles)
BARIATRIC SURGERIES
- Laparoscopic Sleeve Gastrectomy
- Laparoscopic Gastric Bypass
HEPATOBILIARY-PANCREATIC SURGERIES
- Complicated liver resections for liver tumors and Haemangiomas, Hepaticojejunostomies, Choledochal Cyst Surgery etc.
- Portacaval and Splenorenal Shunt Operations for Portal Hypertension.
- Complicated Biliary Stricture Surgeries and major Pancreati c Resections like Whipples, Lateral Pancreaticojejunostomy for Chronic Pancreatitis.
GALLBLADDER
- Gallbladder is a pear shaped organ present close to the liver
- Its function is to store and concentrate bile juice produced by liver.
- Bile is a liquid produced by the liver which helps the body to digest fat.
Risk factors
- Gender: Women age between 20 and 60 are twice a likely than men
- Age: All age groups, common in the 30-40 years
- Obesity
- Excess Estrogen (women on oral contraceptive pills etc.)
- Cholesterol-lowering drugs
- Diabetes
- Rapid weight loss
- Prolonged fasting
- Hereditary blood disorders
- Unknown Geological factors, common in northern and eastern part of india.
What are the symptoms?
- Unknown Geological factors, common in northern and eastern part of india.
- Severe Abdominal pain in right upper abdomen, occur suddenly
- Attacks follow fatty meals, occur during night
- Pain in the back between the shoulder blades & right shoulder
- Nausea or vomiting
- Fever With Chills
- Abdominal bloating (Gas formation)
- Belching
- Indigestion
- Sweat
- Yellowish colouration of skin or whites of the eyes
- Clay-coloured stools
- Many people with gallstones have no symptoms
What complications can these stones cause?
- Recurrent severe abdominal pain or vomiting
- Pus formation in the gallbladder (Empyema)
- Cholangitis
- Gangrene and perforation of the gallbladder
- Acute pancreatitis due to stone sliping
- Jaundice
- Associated with cancer of gallbladder in the long term
What is the treatment?
Medical
-
- Treatment of symptoms of pain with injectable or oral painkillers. No medical therapy is available for gallstones as such which can cure the disease. Though, injectable or oral antibiotics and supportive medications are available for treating the infection.
Surgery:
- Surgery to remove the gallbladder (cholecystectomy) is the only way to treat gallstones. Open method or laparoscopic method which is now the ‘Gold standard’.
Points to remember:
- Gallstones form when substances in the bile juice get precipitated
- Gallstones are common among women and people who are overweight
- Gallstone attacks often occur after eating fatty meals
- Accurate diagnosis is important because symptoms can point towards other problems, including heart attack. Diagnosis can be made in majority of te patients by simple untrasound conducted in a fasting state.
- Gallstones can cause serious problems if they become trapped in the bile ducts such as jaundice and pancreatitis
- Laparoscopic surgery to remove the gallbladder is now the ‘Gold Standard’ for treating gallstones.
- Open surgery for renewal of Gall Bladder for complicated Gallbladder problems.
- This surgery can be done in practically all the patients including patient with a previous abdominal operation / cardiac history / asthma / diabetes etc.
What is obesity?
Obesity is defined as having a body mass index (BMI) of 30 or more. BMI is a measure of your weight in relation to your height. Class 1 obesity means a BMI of 30 to 35, Class 2 obesity is a BMI of 35 to 40, and Class 3 obesity is a BMI of 40 or more. Classes 2 and 3, also known as severe obesity, are often hard to treat with diet and exercise alone.
What is bariatric surgery?
Bariatric surgery is an operation that helps you lose weight by making changes to your digestive system. Some types of bariatric surgeries make your stomach smaller, allowing you to eat and drink less at one time and making you feel full sooner. Other bariatric surgeries also change your small intestine—the part of your body that absorbs calories and nutrients from foods and beverages.
Bariatric surgery may be an option if you have severe obesity and have not been able to lose weight or keep from gaining back any weight you lost using other methods such as lifestyle treatment or medications. Bariatric surgery also may be an option if you have serious health problems, such as type 2 diabetes or sleep apnea, related to obesity. Bariatric surgery can improve many of the medical conditions linked to obesity, especially type 2 diabetes.
HAEMMOROIDS
- Haemmorroids are swollen blood vessels in or around the anus and rectum.
- The haemorrhoidal veins are located in the lowest part of the rectum and the anus.
- Sometimes they swell so that the vein walls become stretched, thin, and irritated by passing bowel movements. Haemorrhoids are classified into two general categories: internal and external
What Causes Hemorrhoids?
- Straining during bowel movements is a primary cause. (A diet low in fiber can result in constipation, which in turn encourages the tendency to strain during bowel movements.)
- Pregnancy, childbirth, heavy lifting and obesity increase the risk of hemorrhoids.
- Prolonged standin g or sitting may be causes.
- Loss of muscle tone due to old age, an episiotomy, or rectal surgery can promote hemorrhoids.
- Digestive problems such as diarrhea and constipation can cause hemorrhoids.
- Excessive consumption of alcohol and caffeine
Symptoms:
- Anal bleeding and pain of any sort is alarming and should be evaluated; it can indicate a life-threatening condition, such as colorectal cancer
- Haemorrhoids are the main cause of anal bleeding and are rarely dangerous, but a definite diagnosis from your doctor is essential.
- Bright red blood on the toilet paper, the stool, or in the toilet bowl after a bowel movement
- Pain, especially during bowel movements
- Anal itching
- Mucus discharge from the anus
- Swelling or a hard lump near the anus area
Who can get haemmorroids?
- Anyone at any age can be affected by haemorrhoids.
- Anyone at any age can be affected by haemorrhoids.
- They are very common, with about 50% of people experiencing them at some time in their life. However, they are usually more common in elderly people and during pregnancy.
- Researchers are not certain what causes haemorrhoids. “Weak” veins – leading to haemorrhoids and other varicose veins – may be inherited.
- The pressure can be caused by obesity, pregnancy, standing or sitting for long periods, straining on the toilet, coughing, sneezing,vomiting, and holding your breath while straining to do physical labour.
- Diet has a pivotal role in causing – and preventing – haemorrhoids.
Preventions:
- A high-fiber diet including fresh fruit, vegetables, and whole-grain breads and cereals is recommended. Consuming Psyllium fiber supplements can also increase your fiber intake.
- Drink plenty of water.
- Don’t strain during bowel movements or stay on the toilet longer than necessary.
- Exercise regularly.
- Do not take laxatives, except bulk-forming laxatives such as Metamucil, Fiberall etc. Other forms of laxatives can cause diarrhea, which can worsen hemorrhoids.
Diagnosis
- Patient history and examination of the anus and rectum are necessary. A doctor may detect internal hemorrhoids with a special scope.
- Barium enema x-rays may be ordered.
How to Treat Hemorrhoids
- Wash the anal area gently but thoroughly after each bowel movement, using a soft tissue and warm water. To dry, dab the area with a soft cloth.
- For external hemorrhoids, apply an ice compress
- Frequent warm baths or sitz baths can relieve mild symptoms of pain and itching.
- Anesthetic ointment and topical corticosteroids (such as hydrocortisone) may ease pain and swelling.
- An injection of a solution that turns the hemorrhoid to scar tissue may be used (sclerotherapy).
- Some hemorrhoids may be tied off using a rubber band (rubber band ligation).
- To help relieve pain use acetaminophen (one brand name: Tylenol), ibuprofen (one brand name: Motrin) or aspirin.
- In severe cases surgical removal (hemorrhoidectomy) may be necessary.
When to Call a Doctor
- Any sign of rectal bleeding should be evaluated by a physician.
- If other symptoms do not improve with home treatment, see a doctor.
APPENDIX
- The appendix (or vermiform appendix; also cecal [or caecal] appendix; vermix; or vermiform process) is a blind-ended tube connected to the cecum, from which it develops in the embryo. The cecum is a pouchlike structure of the colon, located at the junction of the small and the large intestines.
- The term “vermiform” comes from Latin and means “worm-shaped.”
- The appendix has been called a vestigial organ.
- The human appendix averages 9 cm in length but can range from 2 to 20 cm. The diameter of the appendix is usually between 7 and 8 mm. The longest appendix ever removed was 26 cm long. The appendix is usually located in the lower right quadrant of the abdomen, near the right hip bone. The base of the appendix is located 2 cm beneath the ileocecal valve that separates the large intestine from the small intestine. Its position within the abdomen corresponds to a point on the surface known as McBurney’s point.
- The appendix is connected to the mesentery in the lower region of the ileum, by a short region of the mesocolon known as the mesoappendix.
Symptoms of Appendix
- Dull pain near the navel or the upper or lower abdomen that becomes sharp as it moves to the lower right abdomen; this is usually the first sign, but it occurs in less than half of appendicitis cases.
- Loss of appetite
- Nausea or vomiting soon after abdominal pain begins
- Abdominal swelling
- Abdominal swelling
- Temperature of 100 to 101 degrees Fahrenheit
- Constipation or diarrhea with gas
- Inability to pass gas
- In many cases, atypical symptoms appear, including:
- Dull or sharp pain anywhere in the upper or lower abdomen, back, or rectum
- Painful urination
- Vomiting that precedes the abdominal pain
What causes Appendix?
- Vomiting that precedes the abdominal pain
- It’s not always clear what causes appendicitis, and while there seems to be some correlation with a family history, there’s no way to know if or when you might get appendicitis. The condition often arises from one of two issues: A gastrointestinal infection (viral, bacterial, or fungal) that has spread to the appendix, or an obstruction that blocks the opening of the appendix.
- In the second case, there can be several different sources of blockage. These include:
- Lymph tissue in the wall of the appendix that has become enlarged
- Hardened stool, parasites, or other growths
- Irritation and ulcers in the gastrointestinal tract
- Abdominal injury or trauma
- Foreign objects, such as pins, stones, or bullets
- Air pollution has also been linked to an increased risk for appendicitis. Scientists suspect that high levels of ozone might increase inflammation in the intestine or increase susceptibility to infection.
How is appendix diagnosed?
- Your doctor will begin by performing a physical exam. They will look for tenderness in the lower right quadrant of your abdomen. If you’re pregnant, the pain may be higher. If perforation occurs, your stomach may become hard and swollen.
- There isn’t any one test to diagnosis appendicitis. First, your doctor will order a complete blood count (CBC) test. A CBC can determine if there’s a bacterial infection. Bacterial infection is often correlated with appendicitis.
- Your doctor will also perform several tests to rule out other similar conditions:
- Urinalysis can rule out a urinary tract infection or kidney stone.
- Pelvic exams can make certain that you aren’t experiencing any reproductive problems. They can also rule out other pelvic infections.
- Pregnancy tests can rule out a suspected ectopic pregnancy.
- Abdominal imaging can determine if you have an abscess or other complications. This may be done with an X-ray, ultrasound, or CT scan.
- Chest X-ray can rule out right lower lobe pneumonia. This sometimes has symptoms similar to appendicitis.
- If your doctor is unable to pinpoint another cause for your symptoms, you will be diagnosed with appendicitis.
What are the treatment options for appendix?
- Treatment for appendicitis varies. In most cases, however, surgery will be necessary. The type of surgery will depend on the details of your case.
- If you have an abscess that hasn’t ruptured, your doctor may first administer antibiotics. Your doctor will then drain the abscess using a tube placed through your skin. After you’ve received treatment for the infection, you’ll undergo surgery to remove your appendix.
- If you have a ruptured abscess or appendix, surgery may be necessary right away. Surgery to remove the appendix is known as an appendectomy.
- Your doctor can perform this procedure as open surgery or through a laparoscopy. Laparoscopy is less invasive, making the recovery time shorter. However, open surgery may be necessary if you have an abscess or peritonitis. In rare cases, appendicitis may get better without surgery. This is only an option if your abdominal pain is minimal and your diagnostic tests are normal. In this scenario, your treatment plan might only involve antibiotics and a liquid diet until your symptoms resolve.
What is a hernia?
A hernia is a weakness or tear the abdominal muscles that allows organs, such as intestines or fatty tissue, to protrude through the weakened area. This can cause a noticeable bulge under the skin as well as pain and discomfort. Symptoms can feel worse when you stand for long periods, or on strain your abdominal muscles such as when lifting heavy objects.
What causes a hernia?
Many hernias are the result of a defect or weakness in the abdominal wall that was present at birth. The area can be weakened by age or injury and can especially be weakened by a previous surgical incision. Although some hernias are more common in men, they can develop in anyone. Riskfactors for a hernia include:
- Chronic cough
- Smoking
- Obesity
- Straining while lifting heavy objects
- Straining during bowel movements or urination
- Pregnancy
- Certain medications such as steroids.
Types of Hernia
All hernias are not created equal. They are characterized by their location in the abdominal wall and occasionally by their specific cause. There are three types of hernias:
- 1. Inagural Hernia:An inguinal hernia is the most common type of hernia.Inguinal hernias occur in men about five times more frequently than in women due to a potential weak spot in the groin when a male’s testicles descend during fetal development. An indirect inguinal hernia is the type of hernia that develops in this weak spot. The hernia may then descend into the scrotum in men or, in women, to the outer folds of the vagina. A direct inguinal hernia is less common and occurs very near the indirect inguinal hernia in the groin.
- 2. Umbilical hernia:An umbilical hernia occurs in the naturallyweakened area of the navel or belly button where the umbilical cord was attached.These are frequently seen in children, but are also often seen in adults. In small children, umbilical hernias will usually fade away as the child ages. In adults, the only way to treat an umbilical hernia is through surgery.
- 3. Incisional hernia:An incisional hernia is located at thesite of a previous surgical incision. Any area where someone has had surgery will remain somewhat weakened through out his/her lifetime. Hernias can develop in these incisions during the weeks, months or even years after the initial operation. There are many factors that can affect the formation of an incisional hernia including smoking, weight, other medical problems and the type of healing tissue the patient naturally develops after a surgical incision.
Hernia Repair Techniques
Several hernia repair techniques are available for patients: suturing A few muscular defects can simply be sutured closed with good results. Most,however, require more. Mesh is a piece of prosthetic material. The mesh is inserted through an incision in the abdomen or groin and sutured into position. The placement of a mesh helps reduce tension on the wound, reduce the chance of recurrence of the hernia and reduce pain.
- Laparoscopic placement of mesh:This technique is often described as aminimally invasive approach. It requires three or four small incisions. The mesh is secured below the abdominal muscles and hernia. Each technique has its benefits and it is important to have several options when choosing a repair technique.
- Open repair:laparoscopic repairPlastic surgery As the problem of obesit increases in the general population, we see individuals with exceptionally large hernias and extensiveover-hanging skin; its removal is essential to decrease the pull on the abdominal wall and the incidence of recurrent hernias. In such cases, a combined approach with plastic surgery is performed to excise these large aprons of skin. Muscle flaps are also occasionally used in reconstructing theabdominal wall.
- The Consult:The patient is first seen by the general surgeons to plan the operation.
